ASPIRE Educational Series: Myasthenia Gravis (MG)- Part 7
Myasthenia gravis is a chronic autoimmune neuromuscular disease characterized by varying degrees of weakness of the skeletal (voluntary) muscles of the body. It occurs when communication between nerve cells and muscles (the neuromuscular junction) becomes impaired. According to the Myasthenia Gravis Foundation of America, MG is the most common primary disorder of neuromuscular transmission.
MG is a relatively rare condition that affects between 14 and 20 out of every 100,000 people in the United States. Although the disorder usually becomes apparent during adulthood, symptom onset may occur at any age. It most commonly affects young adult women (under 40) and older men (over 60). Myasthenia gravis is not directly inherited nor is it contagious. Occasionally, the disease may occur in more than one member of the same family.
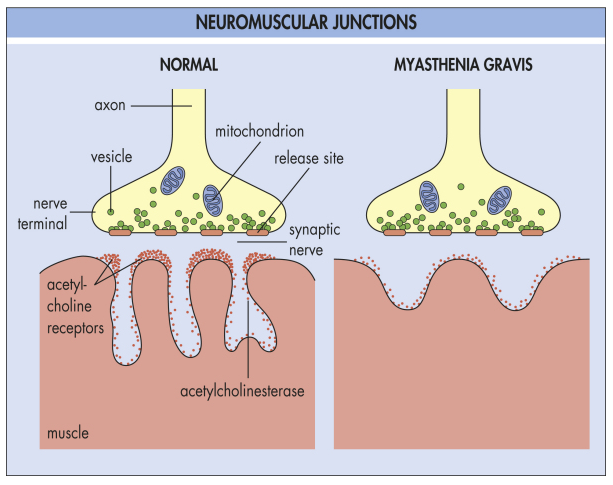
The nerves communicate with muscles by releasing chemicals called neurotransmitters that fit precisely into receptor sites on the muscle cells at the neuromuscular junction. In Myasthenia gravis, the body’s own immune system produces antibodies that block and destroy many of the muscles receptor sites for the neurotransmitter called acetylcholine. The antibodies destroy the receptor sites more rapidly than the body can replace them. This impairment prevents crucial muscle contractions from occurring, resulting in muscle weakness. Another antibody was identified that attacks the muscle specific kinase protein (MuSK). These anti-MuSK antibodies also lead to a decrease in the number of acetylcholine receptors. Recently, antibodies to LRP-4 (lipoprotein receptor protein 4) were identified in patients without antibodies to MuSK or AChR. Whether these antibodies cause disease has not been absolutely confirmed.
The exact cause of this autoimmune reaction is unclear. One theory is that certain viral or bacterial proteins may prompt the body to attack acetylcholine. There’s also evidence that an immune system gland called the thymus plays a role in MG. Located in the chest just below the throat, the thymus is essential to the development of the immune system. About 15% of people with MG have a thymic tumor, called a thymoma, and another 65% have overactive thymic cells, a condition called thymic hyperplasia. When the thymus doesn’t work properly, the T cells might lose some of their ability to distinguish self from non-self, making them more likely to attack the body’s own cells.
Symptoms of MG may be variable, with disease involvement potentially localized to certain muscles or affecting multiple muscle groups. The disease may be limited to certain eye muscles (Ocular myasthenia gravis. The disorder often starts with weakness in the eye muscles leading to drooping of the upper eyelids (ptosis) and double vision (diplopia). In generalized MG, affected individuals may develop muscle weakness in the face, jaw and throat area. This bulbar weakness — named for the nerves that originate from the bulblike part of the brainstem and may cause swallowing (dysphagia) and speaking (dysarthria) difficulties. It also can lead to frequent choking spells, and make eating unpleasant and tiresome. It may also affect limb muscles, making it difficult to lift the arms over the head, rise from a sitting position, walk long distances, climb stairs or grip heavy objects. In some cases, weakness may spread to muscles in the chest that control breathing. Weakness and fatigue in MG tend to fluctuate from day to day, and even during a single day. People with the disease are often strongest in the morning after a full night’s sleep and weakest in the evening.
Diagnosis is done by reviewing symptoms, medical history and physical examination. Several tests may be conducted including:
- Neurological examination: by testing reflexes, muscle strength, muscle tone, senses of touch and sight, coordination and balance.
- Edrophonium test: Injection of the chemical edrophonium chloride (Tensilon) may result in a sudden, although temporary, improvement in your muscle strength. This is an indication that one may have myasthenia gravis. Edrophonium chloride blocks an enzyme that breaks do acetylcholine, the chemical that transmits signals from your nerve endings to your muscle receptor sites.
- Ice pack test: In this test, a doctor places a bag filled with ice on your eyelid. After two minutes, your doctor removes the bag and analyzes your droopy eyelid for signs of improvement. Doctors may conduct this test instead of the edrophonium test.
- Blood analysis: to reveal the presence of abnormal antibodies that disrupt the receptor sites where nerve impulses signal your muscles to move.
- Repetitive nerve stimulation: To diagnose myasthenia gravis, doctors will test the nerve many times to see if its ability to send signals worsens with fatigue.
- Single-fiber electromyography (EMG)
- Imaging scans: CT scan or an MRI to check if there’s a tumor or other abnormality in the thymus.
- Pulmonary function tests
Although there is no cure for MG, there are several therapies available to help reduce and improve muscle weakness. Medications used to treat the disorder include anticholinesterase agents such as neostigmine and pyridostigmine, which help improve neuromuscular transmission and increase muscle strength. Immunosuppressive drugs such as prednisone, azathioprine, cyclosporin, mycophenolate mofetil, and tacrolimus may also be used. These medications improve muscle strength by suppressing the production of abnormal antibodies. Their use must be carefully monitored by a physician because they may cause major side effects. Thymectomy, the surgical removal of the thymus gland (which often is abnormal in individuals with myasthenia gravis), reduces symptoms in some individuals without thymoma and may cure some people, possibly by re-balancing the immune system. Thymectomy is recommended for individuals with thymoma. Plasmapheresis, or plasma exchange, may be useful in the treatment of MG also. This procedure removes the abnormal antibodies from the plasma of the blood. The improvement in muscle strength may be striking, but is usually short-lived, since production of the abnormal antibodies continues. When plasmapheresis is used, it may require repeated exchanges. Intravenous immune globulins (IVIg) are sometimes used to affect the function or production of the abnormal antibodies also.
References
- Myasthenia Gravis. NORD – National Organization for Rare Disorders. www.rarediseases.org/rare-diseases/myasthenia-gravis/ Retrieved on 23-01-17.
- Myasthenia Gravis – Signs and symptoms. MDA – Muscular Dystrophy Association. www.mda.org/disease/myasthenia-gravis/signs-and-symptoms . Retrieved on 23-01-17.
- Myasthenia gravis – Diagnosis. NHS UK. www.nhs.uk/Conditions/Myastheniagravis/Pages/Diagnosis.aspx. Retrieved on 23-01-17.
- Myasthenia gravis. Mayo Clinic – Patient care & health information. www.mayoclinic.org/diseases-conditions/myasthenia-gravis/diagnosis-treatment/. Retrieved on 23-01-17.
- Myasthenia Gravis. MedlinePlus. www.medlineplus.gov/myastheniagravis.html. Retrieved on 23-01-17.
- Treatment for MG. MGFA – Myasthenia Gravis Foundation of America Inc. www.myasthenia.org/WhatisMG/TreatmentforMG.aspx. Retrieved on 23-01-17.
- Myasthenia Gravis Fact Sheet. NIH – National Institute of Neurological Disorders and Stroke. www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Myasthenia-Gravis-Fact-Sheet. Retrieved on 23-01-2017.
- Myasthenia Gravis. Medscape. www.emedicine.medscape.com/article/1171206-overview. Retrieved on 23-01-2017.
- Myasthenia Gravis Highlights. Healthline. www.healthline.com/health/myasthenia-gravis#Overview. Retrieved on 23-01-17.